Many health conditions can benefit from rehabilitation. This can reduce the impact of these conditions on a person’s daily life.
For example, pulmonary rehabilitation plans help to clear excess sputum from the lungs, reducing the likelihood of infections and improving breathing ability.
Physiotherapists work with doctors and other health professionals to provide care. They also work with patients and their families and caregivers to improve quality of life and movement abilities.

Strengthening
Physiotherapy is highly effective in alleviating pain caused by injuries, musculoskeletal conditions and chronic issues. Physiotherapists use a combination of manual therapy techniques and therapeutic exercises to reduce pain and help patients return to their normal lives. This can reduce the reliance on medications and avoid more invasive treatment options.
Many people in low and middle-income countries are living with health conditions that require rehabilitation, but their needs are not being met. This gap is largely due to inadequate advocacy strategies, limited political support, and weak and under-utilized referral pathways.
Rehabilitation is an important part of primary healthcare (PHC), as it helps individuals manage their health conditions and improve their quality of life. It promotes healthy lifestyles, and helps individuals stay active and independent in their daily activities.
Moreover, physiotherapy can help reduce the risk of disability by addressing specific physical and mental problems like depression, anxiety and loneliness. Physiotherapists can also develop treatment plans that incorporate a variety of interventions, including acupuncture, massage and exercise.
Physiotherapy is an essential service that should be available to everyone who requires it. Regardless of age, ethnicity, or socioeconomic status, OH! physiotherapy ensures that everyone has a right to access rehabilitation services, especially when they are needed the most. By improving access and quality of rehabilitation, we can ensure that all individuals have the opportunity to achieve their full potential, live longer, healthier lives, and enjoy a better quality of life.
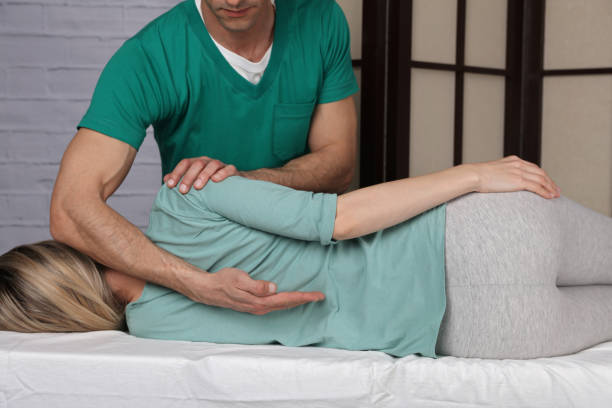
Stabilization
A primary goal of physiotherapy is to improve function, mobility and stability through manual techniques. This includes stretching exercises and joint mobilization to restore a normal range of motion and flexibility.
The central ‘core’ muscles are an important part of the body’s ability to control movement and stabilize the spine. Physical therapists teach patients to consistently perform core strengthening programs that increase their strength and improve balance and posture.
Many injuries are caused by poor posture and other ergonomic factors. Physiotherapists provide advice, education and guidance on the best ways to improve your posture and work habits.
Physiotherapy also helps you manage your symptoms so that you can live a full and active life. This can include addressing underlying health conditions, improving your daily activities, educating you to self-manage your condition, providing assistive products and ensuring you have the support you need.
Rehabilitation, is an essential health service for anyone with a chronic illness or injury. It reduces the need for hospitalization, shortens stays in hospitals and minimizes re-admissions. It enables people to be as independent as possible in their everyday lives and to participate in activities, work and community roles. It also improves their quality of life and reduces social isolation and depression. It is an essential element of universal health care and should be available to everyone

Prevention
When physiotherapists aren’t helping people recover from injuries, they’re working to prevent them from happening in the first place. They’re movement experts who can identify biomechanical imbalances, weak muscles or faulty movement patterns that could lead to injury.
Physiotherapy can also help reduce the impact of health conditions by providing self-management strategies and assistive devices. This is especially important for chronic health conditions, which can have a devastating effect on the quality of life and independence.
For example, a physiotherapist can perform a balance and fall risk assessment and provide customized treatment plans including exercises that can improve strength and mobility and reduce the risk of falling. Falls are common among elderly people and can have serious consequences, but they’re also preventable.
Physiotherapy is also an excellent way to prepare for physical activities like sports or work. By improving strength, mobility and function, individuals can be more confident in their abilities and minimize the risk of injuries. This translates into better performance and a more positive overall experience. Whether you’re an amateur athlete or work in a physically demanding job, preventing injuries is vital to keep you healthy and happy. Physiotherapists are the best choice for injury prevention because they know how to spot potential problems before they occur. Think of your physiotherapist as a body mechanic – get them in before the damage is done!
Education
Physiotherapists and podiatrists at Optimise Health are in the position to educate patients on physical health, movement patterns, and lifestyle factors. This can help patients improve and maximise their quality of life and movement potential. In this way, they provide patients with a holistic approach to healthcare and rehabilitation.
Education in physiotherapy also involves teaching people how to prevent injuries and maintain their physical health. This can be done through a combination of clinical examinations, patient histories, and specialized tests that measure strength, movement patterns, balance, and overall functional ability. Physiotherapists can teach patients proper body mechanics, posture, and exercise techniques that will reduce the risk of injury.
In some cases, physiotherapists work closely with doctors and other healthcare professionals to ensure that a patient receives the best care possible. They may be employed in a clinic, hospital, nursing home, rehabilitation facility, or even at the patient’s home.
Physiotherapy training is governed by legal and regulatory frameworks that vary from country to country. These frameworks establish guidelines and standards for the practice of physiotherapy, ensuring patient safety and adherence to professional codes of conduct. However, a number of studies have shown that undergraduate physiotherapy programmes lack sufficient mental health content. This needs to be rectified in order for physiotherapists to be better equipped to manage patients with SMI. A structured service learning programme can enhance a student’s ability to provide effective treatment to individuals with SMI and also encourage a positive attitude towards mental illness.