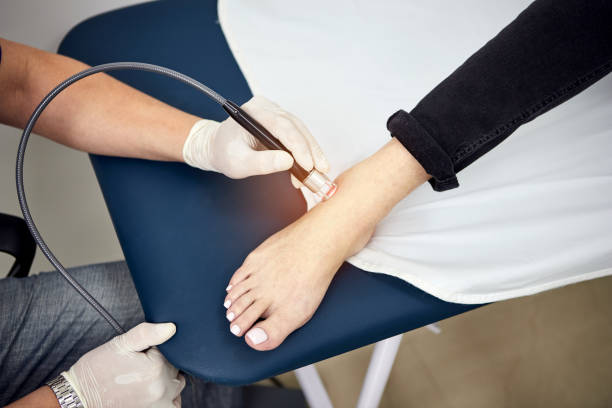
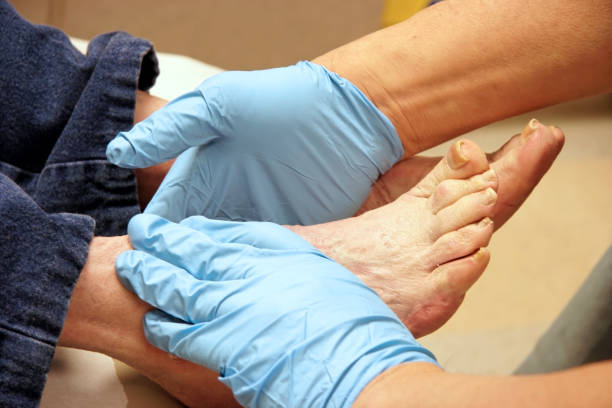
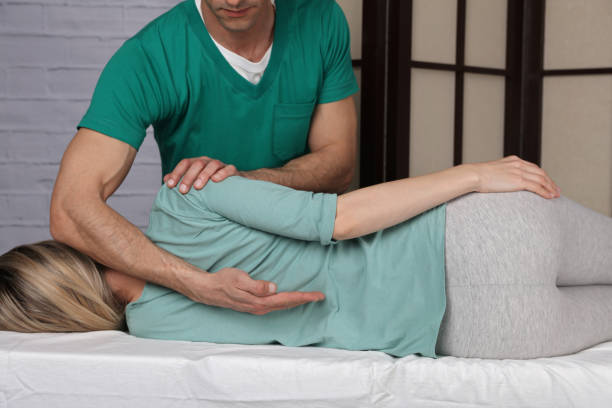
Podiatrists are the specialists in the foot and ankl. They are trained in biomechanics, gait analysis, podiatric orthopaedics, pharmacology, and general medical practice.
Change can be challenging for clinicians. Changing professional practice can challenge beliefs, values and attitudes that define the current practice. Lewin suggests there are three stages in the process of change.

Orthotics
Podiatrists can help reduce foot pain by prescribing orthotics. These shoe inserts help redistribute pressure on the feet, and are designed to fit inside your shoes. They can be purchased ‘off the shelf’ or custom made from a plaster cast or digital picture of your foot. Orthotics are often recommended for people with chronic foot problems, such as calluses or bunions. They can also be beneficial for athletes who need to maximise performance.
Podiatry centre near Prospect can help reduce foot pain by prescribing orthotics. These shoe inserts help redistribute pressure on the feet, and are designed to fit inside your shoes. They can be purchased ‘off the shelf’ or custom made from a plaster cast or digital picture of your foot. Orthotics are often recommended for people with chronic foot problems, such as calluses or bunions. They can also be beneficial for athletes who need to maximize performance.
Some patients may be referred to podiatry by their general practitioner for management of foot problems and injuries. Medicare can cover podiatrist services to Unley for these patients if they have a chronic disease management (CDM) plan.
The word podiatry was adopted to avoid confusion with chiropodists and chiropractors in the US, and is composed of the Greek roots “pod” meaning feet and “iatros” meaning physician. It is a more accurate and up-to-date term for the profession that has come to be recognized as an integral part of medical care. Podiatrists are medically trained to diagnose and treat problems with the feet, ankles and lower leg, and use advanced technology to assess how your feet work while you move. They listen carefully to your complaints, and take the time to fully evaluate your foot health. They also perform routine nail care, remove calluses and corns, and provide treatment for common conditions such as diabetes, arthritis and sports injuries.
Biomechanics
Podiatrists study the structure of the feet and lower legs as well as their function. This includes the way in which muscles, bones and joints work together to absorb and propel impact during movement. This knowledge is used to diagnose and treat a wide variety of podiatric conditions.
The large external forces that our feet and lower extremities endure during daily weight-bearing activities are likely to be the root cause of most of the clinical pathologies podiatrists encounter. This makes biomechanics a natural topic to explore. Doug Richie notes that although podiatric journals have monthly articles on joint moments, gait analysis, muscle function and pathomechanics of injury, podiatric biomechanics is no longer taught extensively in podiatric medical schools.
To do so will require a paradigm shift in thinking. Changing the way we view our patient’s roles and how we deliver care requires us to unfreeze our beliefs, values, attitudes and assumptions. This is the first step to creating a culture of change. Then, podiatry can take advantage of the numerous tools and technologies available to improve foot health and wellbeing for everyone. We can use telemedicine, for example, to help patients with their aches and pains without the need to travel to a podiatrist.
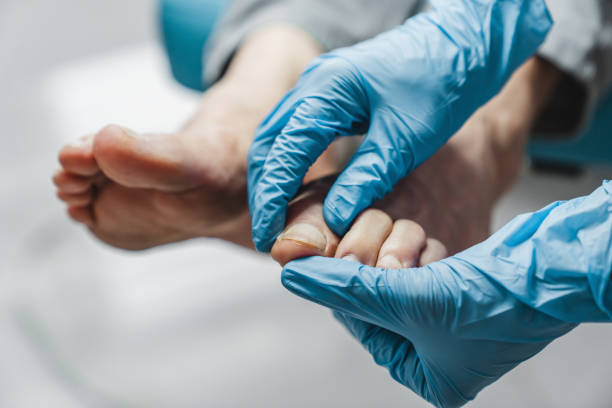
Surgery
Podiatric surgery is a specialist sub-specialty that requires extensive post graduate medical and surgical training. It is an approved specialty recognised by Australian state and federal governments and included in the health insurance rebate system. Podiatric surgeons are qualified to surgically manage foot and ankle pathology. They have an excellent level of ‘differential diagnosis’ and use medical imaging strategically to augment their clinical findings. Podiatric surgery can be used to treat a number of conditions including foot biomechanics, deformities, infections, trauma, overuse, sports injuries and nerve injury (neuropathic pain).
During the 1960’s and 1970’s the podiatry profession developed a significant public health presence through podiatric community based projects such as the Queensbridge Health Maintenance Project in New York City. This was an innovative community health initiative in a housing authority development that provided podiatric care to an older population living at poverty levels.
The current landscape of healthcare delivery and podiatry’s position within it is changing. There is a need to improve the ability of podiatrists to adapt to change at the practice, professional and organisational levels. This can be achieved by encouraging an open learning culture where successful attempts at change are shared. It is also important to develop a more effective approach to the implementation of change that will allow podiatrists to embrace it and thrive in future healthcare delivery.
Nutrition
Podiatrists are increasingly being commissioned to help address societal issues such as poor diet and obesity. This reflects the current trend within healthcare towards helping people to live more healthily and therefore avoid or reduce the need for surgery or medication. This means that podiatry has to develop a holistic approach and ensure that patients are getting the right nutrients for good health.
Evidence from the public health field shows that people who are informed, involved, able and confident in self-managing their conditions have better outcomes than those who do not [17,18]. Podiatric medicine can play an important role in patient engagement and facilitating shared responsibility, but this requires a change in professional attitude and practice.
Research has shown that podiatrists cite professional attitude, lack of time, skills and funding as significant barriers to changing their routine clinical practices. Additionally, many practitioners feel that the literature can be too obscure and irrelevant to everyday practice. This can result in podiatrists not searching or reading the literature that could inform their practice.
During the 1960’s, a number of projects in relation to foot health and community health were initiated by podiatric physicians. These included the Philadelphia Department of Health Project Keep Them Walking, the Washington DC Health Department Community Clinical Podiatry Program and the Minnesota Department of Health Nursing Home Study. In January of 1972 the Council on Public Health of APMA recommended that podiatric health be included as a separate section of APHA. This was endorsed by the Board of Trustees at its mid-winter meeting.